Healthcare Claims Management Market Report Scope & Overview:
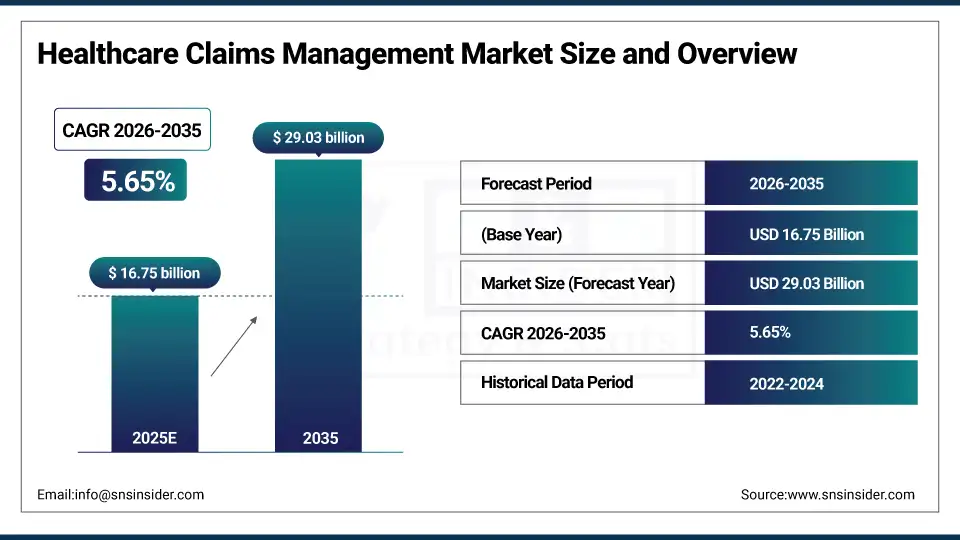
The Healthcare Claims Management Market size was valued at USD 16.75 billion in 2025 and is expected to reach USD 29.03 billion by 2035, growing at a CAGR of 5.65% over the forecast period of 2026-2035.
The global healthcare claims management market trend is a growing demand for automated claims processing solutions such as medical billing software, integrated revenue cycle management platforms, and electronic claims submission systems. The growth of the market is driven by increasing healthcare expenditure, government mandates for healthcare digitization, and rising provider and payer expectations for faster and more accurate claims adjudication. This trend is also driven by a growing adoption of value-based care reimbursement models and the growing focus on reducing claims denials and administrative overhead as healthcare organizations become more focused on improving revenue cycle efficiency and are more willing to invest in cloud-based and AI-assisted claims management technologies, resulting in growth in the domestic and international market for both integrated and standalone healthcare claims management solutions.
For instance, in March 2024, growing regulatory pressure and increased adoption of electronic claims submission standards drove a 19% increase in cloud-based claims management platform deployments across healthcare provider networks in North America, boosting claims processing accuracy and administrative cost reduction.
Healthcare Claims Management Market Size and Forecast:
-
Market Size in 2025E: USD 16.75 billion
-
Market Size by 2035: USD 29.03 billion
-
CAGR: 5.65% from 2026 to 2035
-
Base Year: 2025
-
Forecast Period: 2026–2035
-
Historical Data: 2022–2025
To Get more information On Healthcare Claims Management Market - Request Free Sample Report
Healthcare Claims Management Market Trends
-
Healthcare claims management solutions are being adopted because providers and payers demand faster claims adjudication, real-time eligibility verification, and automated denial management to reduce revenue cycle inefficiencies.
-
Customized medical billing workflows based on payer-specific rules, procedure codes, and compliance requirements to improve first-pass claim acceptance rates and reduce rework costs.
-
The development of AI-powered claims scrubbing tools, robotic process automation (RPA) platforms, and natural language processing systems to improve claims accuracy, reduce manual intervention, and accelerate payment cycles.
-
Electronic remittance advice systems, real-time claims tracking dashboards, and automated prior authorization workflows are all available to ensure continuous revenue integrity and regulatory compliance across provider and payer networks.
-
Increased demand for cloud-based deployment models, mobile-accessible billing interfaces, and self-service claims portals to help improve operational flexibility, data security, and staff productivity.
-
Collaboration between healthcare providers, technology vendors, and health plan administrators to develop integrated claims management ecosystems and improve standards of HIPAA-compliant data exchange and interoperability.
-
CMS, ONC, and HHS promoting standards for electronic data interchange (EDI), ICD-10 compliance, prior authorization reform, and claims transparency to strengthen the regulatory foundation for the market.
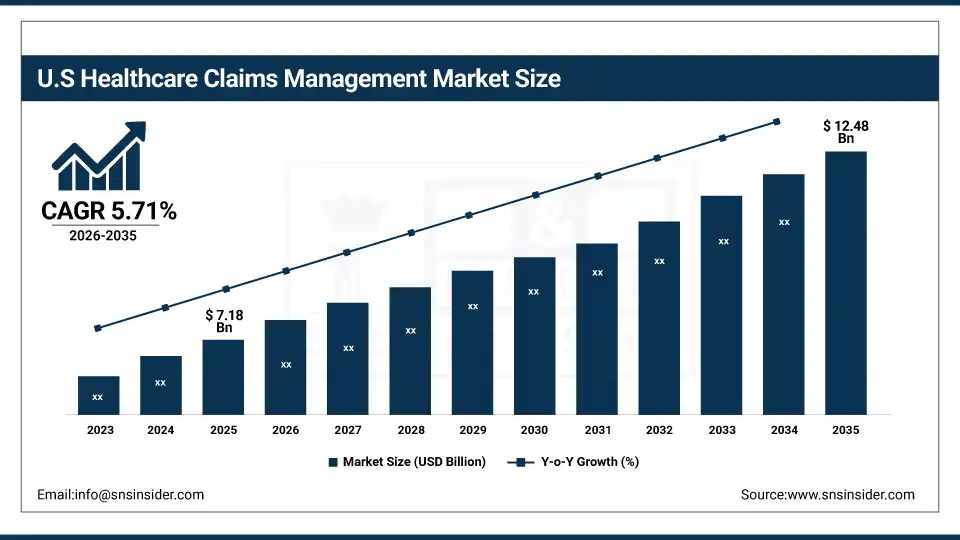
The U.S. Healthcare Claims Management Market was valued at USD 7.18 billion in 2025 and is expected to reach USD 12.48 billion by 2035, growing at a CAGR of 5.71% from 2026-2035. The United States represents the largest market for healthcare claims management, primarily driven by the mandatory adoption of standardized electronic claims formats, federal regulations facilitating interoperable payer-provider data exchange, and a well-developed health IT infrastructure. Government incentives, high health insurance penetration, and increased provider and payer spending on revenue cycle automation technology help to drive growth in the market. Also, the U.S. is the largest regional market in the world, due to the regulatory support and swift adoption of cloud-based and AI-powered healthcare claims management solutions.
Healthcare Claims Management Market Growth Drivers:
-
Rising Administrative Burden and Denial Management Complexity is Driving the Healthcare Claims Management Market Growth
Rising administrative burden and denial management complexity take the center stage as a growth driver for the healthcare claims management market share, and are driven by the increasing volume of insurance claims, growing complexity of payer-specific reimbursement rules, and stringent ICD-10 and CPT coding compliance requirements across professional and institutional billing environments. These pressures for revenue cycle automation and claims accuracy are expanding the base of the market, the penetration of cloud-based and integrated claims processing platforms, and adding to the overall market share globally.
For instance, in June 2024, automated and AI-integrated claims management solutions accounted for ~64% of the total U.S. healthcare provider revenue cycle technology investments, reflecting growing institutional preference for end-to-end claims automation and expanding market share.
Healthcare Claims Management Market Restraints:
-
High Implementation Costs and Legacy System Integration Challenges are Hampering the Healthcare Claims Management Market Growth
High implementation costs and legacy system integration challenges of healthcare claims management platforms also restrict the healthcare claims management market growth, as a large number of healthcare organizations that have access to advanced claims software remain on outdated systems or face significant difficulties migrating data and workflows from legacy billing infrastructure to modern cloud-based or integrated solutions. This might lead to implementation delays, workflow disruption, and reduced return on investment for smaller provider groups and independent practices. As a result, revenue cycle performance suffers and market growth is stunted in regions where health IT investment capacity is limited and claims management expertise is insufficient.
Healthcare Claims Management Market Opportunities:
-
AI and Automation Integration in Claims Processing Drive Future Growth Opportunities for the Healthcare Claims Management Market
The opportunity in AI and automation integration in the healthcare claims management market is in the form of predictive denial prevention, automated prior authorization, and intelligent claims routing. These solutions provide for early identification of billing errors, real-time payer rule updates, and automated claims status monitoring. Through enhanced first-pass resolution rates, reduced days in accounts receivable, and improved operational efficiency, particularly in high-volume hospital and health plan environments, these technologies may improve net revenue capture, reduce administrative costs, and expand the market.
For instance, in April 2024, CMS reported that healthcare organizations actively using AI-powered claims management tools recorded a 21% reduction in claim denial rates and a 16% improvement in clean claim submission rates, highlighting the growing impact of intelligent automation on revenue cycle performance and platform demand.
Healthcare Claims Management Market Segment Analysis
-
By product, claims processing held the largest share of around 58.34% in 2025E, and the medical billing segment is expected to register the highest growth with a CAGR of 6.12%.
-
By component, software dominated the market with approximately 62.47% share in 2025E, while services is expected to register the highest growth with a CAGR of 5.93%.
-
By solution type, integrated solutions accounted for the leading share of nearly 66.81% in 2025E, and standalone solutions is expected to register the highest growth with a CAGR of 6.28%.
-
By deployment mode, cloud-based held the largest share of around 54.62% in 2025E, and web-based is expected to register the highest growth with a CAGR of 6.41%.
-
By end-use, healthcare providers accounted for the leading share of nearly 61.29% in 2025E, and is expected to register the highest growth with a CAGR of 5.84%.
By Product, Claims Processing Leads the Market, While Medical Billing Registers Fastest Growth
The claims processing segment accounted for the highest revenue share of approximately 58.34% in 2025, owing to its central role in payer operations, the high volume of daily claims transactions handled by health plans and clearinghouses, and strong demand for end-to-end electronic claims submission and adjudication workflows. Emerging trends, including increasing automation of eligibility verification and remittance posting and growing regulatory requirements for faster claims resolution. In comparison, the medical billing segment is anticipated to achieve the highest CAGR of nearly 6.12% during the 2026–2035 period, driven by the increasing demand from both professional and institutional billing environments for specialized coding compliance, denial management, and patient billing tools. Drivers include rising adoption among physician groups and hospital outpatient departments, the preference for specialty-specific billing modules, and growing pressure to reduce billing errors and improve patient payment collection rates.
By Component, Software Dominates, while Services Segment Shows Rapid Growth
By 2025, the software segment contributed the largest revenue share of 62.47% due to widespread provider and payer adoption of claims management platforms, billing automation tools, and revenue cycle management suites that reduce manual workload and improve processing accuracy. Growing deployment of SaaS-based claims software coupled with AI-assisted coding and scrubbing capabilities, providers and payers are increasingly dependent on purpose-built software to manage the growing complexity of claims workflows. The services segment is projected to grow at the highest CAGR of about 5.93% between 2026 and 2035 due to growing outsourcing of revenue cycle management, coding, and denial management functions to specialized third-party vendors. Some of the reasons include the shortage of in-house billing expertise, growing demand for managed services among small and mid-sized healthcare organizations, and healthcare organizations' preference for variable-cost service models that reduce the need for internal staffing.
By Solution Type, Integrated Solutions Lead, and Standalone Solutions Registers Fastest Growth
The integrated solutions segment accounted for the largest share of the healthcare claims management market with about 66.81%, owing to strong provider and payer preference for unified platforms that connect claims processing, medical billing, EHR data, and payment posting within a single interoperable workflow. Reasons driving the integrated solutions segment include growing regulatory requirements for seamless payer-provider data exchange, the shift toward value-based reimbursement models that demand end-to-end revenue cycle visibility, and the cost efficiencies achieved by consolidating multiple billing functions onto a single platform. In addition, the standalone solutions segment is slated to grow at the fastest rate with a CAGR of around 6.28% throughout the forecast period of 2026–2035, as smaller practices, specialty clinics, and independent billing companies seek affordable, purpose-specific tools for individual billing or claims functions without the cost of a full integrated suite. Increased focus on niche billing requirements and flexibility in system configuration contribute to their adoption.
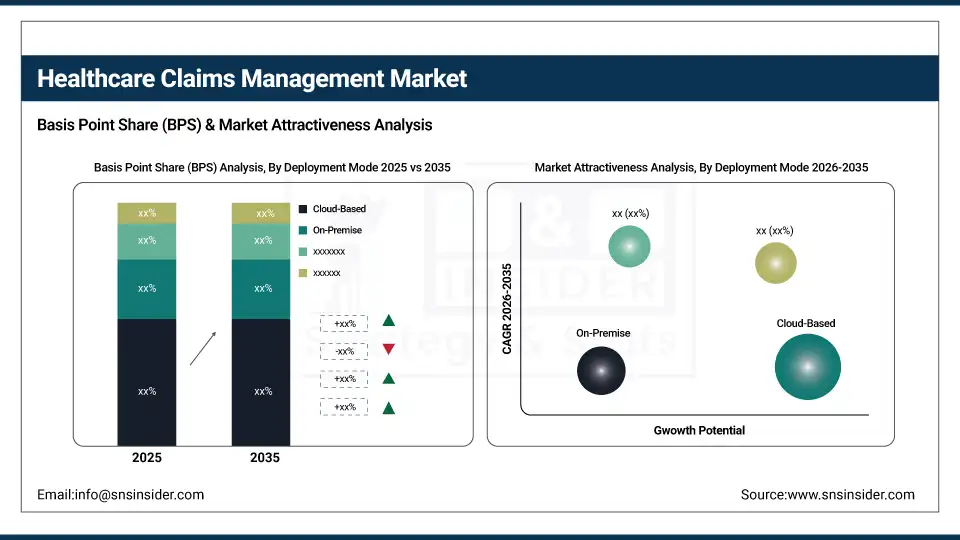
By Deployment Mode, Cloud-Based Leads, and Web-Based Registers Fastest Growth
The cloud-based segment accounted for the largest deployment share of approximately 54.62% in 2025, owing to its scalability, lower upfront IT infrastructure costs, and ability to support real-time claims data access and remote workforce operations. Growing adoption of SaaS-based revenue cycle platforms and increasing awareness of cloud security standards among healthcare organizations are encouraging broader migration from on-premise to cloud-hosted claims management environments. The web-based segment is expected to register the highest CAGR of 6.41% during the forecast period, driven by growing demand for browser-accessible claims platforms that require no local software installation and support multi-device access across provider offices, billing teams, and remote staff. The on-premise segment continues to maintain a steady presence among large hospital systems and government-funded health programs with strict data residency and compliance requirements.
By End-Use, Healthcare Providers Lead, and Registers Fastest Growth
The healthcare providers accounted for the largest share of the healthcare claims management market with about 61.29%, owing to their direct responsibility for submitting accurate claims, managing billing compliance, and collecting patient payments across both professional and institutional care settings. Reasons driving the provider segment include the growing complexity of payer contracting, increasing patient cost-sharing obligations that require more sophisticated patient billing tools, and rising pressure to reduce days in accounts receivable and improve net revenue capture. In addition, it is slated to grow at the fastest rate with a CAGR of around 5.84% throughout the forecast period of 2026–2035, as hospitals, physician groups, and outpatient clinics invest in end-to-end revenue cycle management platforms, prior authorization automation, and denial prevention analytics. Increased focus on reducing claim rework costs and improved patient financial experience drive continued investment.
Healthcare Claims Management Market Regional Highlights:
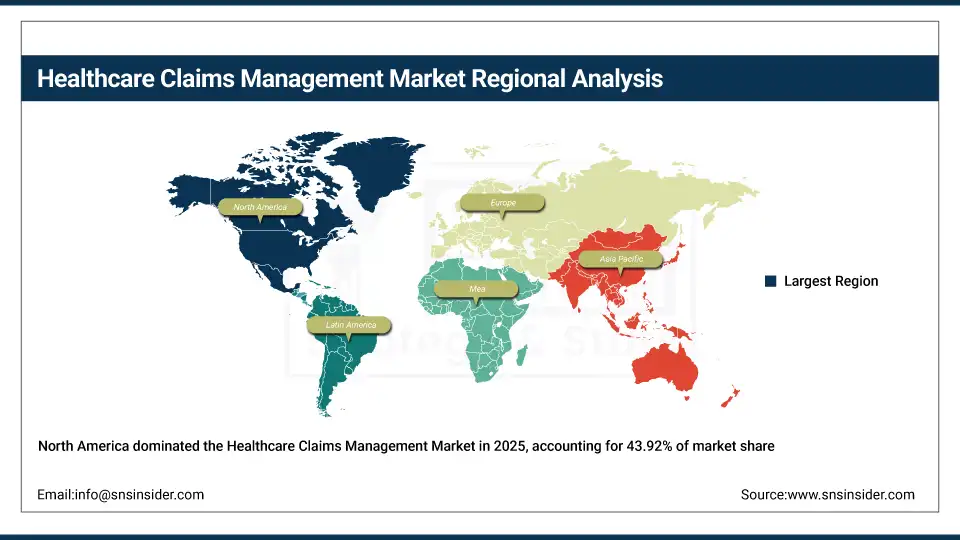
North America Healthcare Claims Management Market Insights:
North America held the largest revenue share of over 43.92% in 2025 of the healthcare claims management market due to an established health IT environment, stringent requirements for standardized electronic claims submission, and increased provider and payer awareness regarding the advantages of automated revenue cycle management. Drivers include ubiquitous use of EHRs, a well-developed clearinghouse infrastructure, growing adoption of AI-assisted billing tools, and greater acceptance of cloud-based claims platforms as operational standards among large health systems and regional providers. At the same time, various government mandates including CMS prior authorization reform requirements and HIPAA EDI compliance standards, and enormous investments in revenue cycle technology from providers and payers, are anchoring healthcare claims management software and services in the market and ensuring multibillion dollar revenues across the region.
Get Customized Report as per Your Business Requirement - Enquiry Now
Asia Pacific Healthcare Claims Management Market Insights:
Asia Pacific is the fastest-growing segment in the healthcare claims management market with a CAGR of 7.18%, as the awareness about digital healthcare administration, government health insurance expansion programs, and healthcare IT modernization efforts across countries such as China, India, Japan, Australia, and South Korea is growing. Factors including rapid expansion of private health insurance coverage, rising middle-class healthcare utilization, and growing deployment of hospital information systems with integrated claims modules are stimulating the market growth. National eHealth initiatives and government-led health insurance digitization programs have been instrumental in standardizing electronic claims submission, especially in economies transitioning from paper-based to fully digital claims workflows. Public-private partnerships and regional government programs also help in advancing healthcare administration efficiency and digital health infrastructure. Increase in demand in the Asia Pacific region owing to rising healthcare expenditure and growing affordability and accessibility of cloud-based claims management platforms.
Europe Healthcare Claims Management Market Insights:
The healthcare claims management market in Europe is the second-dominating region after North America on account of an increase in the adoption of electronic health records, robust data protection regulations including GDPR, and increasing national health system modernization efforts across the UK, Germany, France, and the Netherlands. Rising implementation of national health insurance digitization programs, cross-border healthcare billing directives, favorable government funding for health IT infrastructure projects, and growing payer demand for automated adjudication platforms are also contributing to the sustained growth of the market in leading European countries.
Latin America (LATAM) and Middle East & Africa (MEA) Healthcare Claims Management Market Insights:
In Latin America, and Middle East & Africa, the growing healthcare digitization efforts and increase in internet connectivity with mobile device penetration support the healthcare claims management market growth. The rising popularity of affordable cloud-based claims solutions and multilingual billing platform capabilities, along with government universal health coverage expansion initiatives, will aid healthcare administration efficiency and claims processing accuracy. The increasing urban population and improving healthcare infrastructure in these regions are continuing to encourage market growth.
Healthcare Claims Management Market Competitive Landscape:
Optum (Change Healthcare) (est. 1992) is a leading health services and analytics company that focuses on end-to-end revenue cycle management, claims processing, and payer-provider connectivity solutions. It uses its expansive clearinghouse network and claims data assets to deliver intelligent claims management platforms that improve adjudication accuracy, reduce denials, and accelerate payment cycles for providers and payers nationwide.
-
In February 2025, it expanded its AI-powered claims management suite with enhanced predictive denial prevention and automated prior authorization workflows, targeting large integrated delivery networks and regional health plan organizations across North America.
Cerner Corporation (Oracle Health) (est. 1979) is a well-known global health information technology company focused on EHR-integrated revenue cycle management, claims processing, and medical billing solutions. It invests in interoperable claims management platforms and cloud-based billing automation tools with the hopes of revolutionizing the provider billing experience with faster, more accurate, and regulation-compliant claims submission and adjudication capabilities.
-
In May 2024, launched an enhanced cloud-based claims management platform featuring real-time eligibility verification and automated remittance posting capabilities across North American hospital systems, enhancing clean claim submission rates and reducing days in accounts receivable.
athenahealth, Inc. (est. 1997) is a leading cloud-based healthcare technology provider in the fields of medical billing, claims management, and revenue cycle services for ambulatory and hospital-based care settings. The company's claims management portfolio focuses on automated claims scrubbing, payer rule intelligence, and mobile-accessible billing workflows, and features a strong commitment to regulatory compliance and continuous product innovation to complement a strong market presence among physician practices and health systems.
-
In September 2024, introduced advanced claims analytics and automated denial management features for its athenaClinicals platform, strengthening revenue cycle capabilities and expanding adoption among small to mid-sized medical practices and specialty care providers.
Healthcare Claims Management Market Key Players:
-
Optum, Inc. (Change Healthcare)
-
Oracle Health (Cerner)
-
athenahealth, Inc.
-
Epic Systems Corporation
-
Allscripts Healthcare Solutions
-
McKesson Corporation
-
Availity, LLC
-
Cognizant Technology Solutions
-
Conifer Health Solutions
-
Cotiviti, Inc.
-
eClinicalWorks
-
GE HealthCare Technologies Inc.
-
Inovalon Holdings, Inc.
-
Kareo (Tebra)
-
MEDITECH
-
NextGen Healthcare
-
nThrive (formerly Precyse)
-
Waystar Health
-
Experian Health
-
AdvancedMD
| Report Attributes | Details |
|---|---|
| Market Size in 2025 | US$ 16.75 Billion |
| Market Size by 2035 | US$ 29.03 Billion |
| CAGR | CAGR of 5.65% From 2026 to 2035 |
| Base Year | 2025 |
| Forecast Period | 2026-2035 |
| Historical Data | 2022-2024 |
| Report Scope & Coverage | Market Size, Segments Analysis, Competitive Landscape, Regional Analysis, DROC & SWOT Analysis, Forecast Outlook |
| Key Segments | • By Product (Medical Billing, Claims Processing) • By Component (Software, Services) • By Solution Type (Integrated Solutions, Standalone Solutions) • By Deployment Mode (Cloud-based, On-premise, Web-based) • By End-use (Healthcare Providers, Healthcare Payers) |
| Regional Analysis/Coverage | North America (US, Canada, Mexico), Europe (Eastern Europe [Poland, Romania, Hungary, Turkey, Rest of Eastern Europe] Western Europe] Germany, France, UK, Italy, Spain, Netherlands, Switzerland, Austria, Rest of Western Europe]), Asia Pacific (China, India, Japan, South Korea, Vietnam, Singapore, Australia, Rest of Asia Pacific), Middle East & Africa (Middle East [UAE, Egypt, Saudi Arabia, Qatar, Rest of Middle East], Africa [Nigeria, South Africa, Rest of Africa], Latin America (Brazil, Argentina, Colombia, Rest of Latin America) |
| Company Profiles | Optum, Inc. (Change Healthcare), Oracle Health (Cerner), athenahealth, Inc., Epic Systems Corporation, Allscripts Healthcare Solutions, McKesson Corporation, Availity, LLC, Cognizant Technology Solutions, Conifer Health Solutions, Cotiviti, Inc., eClinicalWorks, GE HealthCare Technologies Inc., Inovalon Holdings, Inc., Kareo (Tebra), MEDITECH, NextGen Healthcare, nThrive (formerly Precyse), Waystar Health, Experian Health, AdvancedMD |
Frequently Asked Questions
Ans: The Healthcare Claims Management Market is expected to grow at a CAGR of 5.65% over the forecast period.
Ans: The Healthcare Claims Management Market size was valued at USD 16.75 billion in 2025 and is expected to reach USD 29.03 billion by 2035.
Ans: Rising Administrative Burden and Denial Management Complexity is Driving the Healthcare Claims Management Market Growth.
Ans: The Claims Processing segment dominated the Healthcare Claims Management Market in 2025.
Ans: North America dominated the Healthcare Claims Management Market in 2025.

